In India the word contraception is used almost synonymously with sterilisation in women.
Sterilisation is done predominately by a small incisionin the post-partum phase (after birth of the baby). The days when this was considered the most reliable method of contraception is long over and LARC (Long Acting Reversible Contraception) is the most commonly used mode worldwide.
Read the conversation with a leading gynaecologist, Dr. Vaishnavi who incidentally holds a diploma with the Faculty of Sexual and Reproductive Health (London) about LARC and its benefits.
Excerpts from the interview…
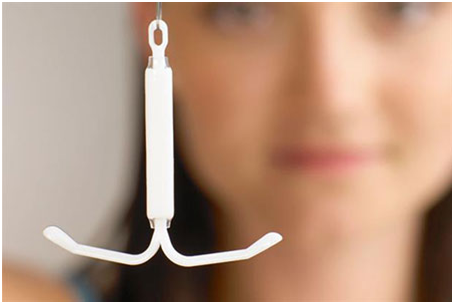
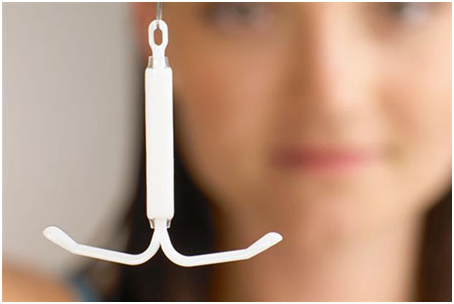
What is LARC?
LARC is Long Acting Reversible Contraception. As the name suggests they work for a longer duration of time, varying from 3 months to 7 years and today’s women who lead extremely busy lives as professionals, homemakers and entrepreneurs etc, do not have to bother about contraception on a daily basis.
Secondly it is reversible, which means if women change their minds about wanting children they can stop this method of contraception and become pregnant again.
Does this involve an operation?
No, it does not in the majority of cases.
I find examinations very intrusive, should I have one to start this kind of contraception?
Not necessarily. Some of these methods involve an injection or an implant in your arm. Your gynaecologist might perform an examination if necessary as part of the initial assessment.
Could you tell me more about these methods?
Sure, it isn’t just one method, there are many types. The commonly used methods are:
- Depot – injection into muscle. This works for three months. It is also useful to treat heavy periods and most women have good relief from their period problems.
- Implanon/Nexplanon – implant inserted in your arm, effective for 3 years. Also recommended for heavy periods. Achieves amenorrhea (no periods) without any ill effects in a large number of patients.
- Mirena-intra-uterine device – inserted into the womb. Effective for 5-7 years. Very effective for period problems and also protects the womb from cancer
- Copper coils – suits women who want to avoid hormones altogether and can be effective for as long as 7 years.
Is it true that the chances of falling pregnant accidentally with these methods are quite high compared to Sterilisation?
No that is a myth – the success rates with the coil and implant are over 99%, even sterilisation is not a 100% foolproof method. The mirena coil especially is touted as more effective than sterilisation, in addition it does not require surgery, and has other health benefits such as protecting the womb against cancer.
Can women with medical problems such as Diabetes and thyroid conditions use these methods?
Yes, it is particularly recommended for women with these medical problems as it protects them from pregnancy until their medical condition is well controlled which is essential to achieve a good outcome for pregnancies complicated by medical problems.
In addition we can use a method, which does not release a large amount of hormone in to the body and blood.
I have heard that this can be harmful for women with cardiac conditions.
In some situations we have to assess the risk and weigh the benefits against the risk. To quote an incident, I had a patient not that long ago with a serious cardiac condition. She had been very ill but got better and neither she nor her physician gave contraception any thought. She got pregnant and became extremely sick because of the effects of the pregnancy on her condition and sadly passed away. This was extremely tragic and could have been prevented.
Are there other conditions where one should have contraception compulsorily?
There are many, to quote a few examples –
- If a woman is on a drug that causes harm to the fetus.
When patients in the reproductive age group (15-45) are started on such drugs they are usually referred to a specialist like myself, by their physicians.
2. Patients with active infections such as Hepatitis and HIV
3. Patients receiving Radiotherapy and Radioactive Iodine.
Can these injections or implants be bought over the counter/or had with our local doctor?
An initial consultation with a specialist is advisable. Once the right contraception for you is initiated you can choose to see your general physician for follow-ups after discussion with your specialist. This is especially advisable if you have any medical or gynaecological problems.
Do any of these have any side effects?
Side effects are minimal and are not experienced by all.
- No periods-this is seen as a benefit by many with irregular periods.
- Weight gain – usually there are other contributing factors
- Bloating and nausea
- Breast tenderness.
If you as a patient are at risk of facing serious side effects, your specialist will advise you to avoid specific methods.
I have heard you can also take these medications if you find yourself pregnant and don’t want to be?
That is not strictly true. You probably mean post coital contraception.
In the event of unprotected intercourse, if the woman approaches us within 24 -72 hrs, post coital contraception can be used to successfully avoid a pregnancy. We commonly use this for condom accidents and abuse victims.
Can most women stop contraception at 40 years of age?
Unfortunately no! This is a dangerous and careless practice. Contraception should be continued until menopause (cessation of periods for a whole year).
Termination of pregnancies (abortion) are risky procedures and can cause physical and emotional trauma. The very idea of reliable contraception is to avoid this and give you complete peace of mind.

Give a Reply