In my clinic at Kauvery Hospital in Chennai, I have an ever increasing number of women who attend requesting a hysterectomy
When I ask them why they think they need a hysterectomy
The answers I get are shocking!
They are;
- My daughter is getting married and I don’t want to bother with contraception or periods for that matter!
- I am not going to have any more children anyways!


- I feel tired all the time; all the doctors I have seen earlier have suggested I have my womb removed.
- My friend has had one and she feels so much better now!
- I read it is a quick and simple operation nowadays
- I don’t want to keep seeing a gynaecologist for this, that and the other
- I have urine leakage
- I have difficulties with sex
- I am tired of my periods
The list goes on and on …
I then have the task of having a discussion with the women to explain why it is not the treatment for all conditions in gynaecology.
The days of offering hysterectomy for every single complaint in a woman are long over.
Hysterectomy is a major operation and while we now have the ability to perform this operation laparoscopically; which allows early and enhanced recovery and discharge home, it is not without risks.
Bleeding during or after surgery is quite common and can be quite severe
Infections if not handled properly can cause significant harm to patients
Bladder and gut injury is quite rare but extremely traumatic for the patient both physically and emotionally
Removal of ovaries before menopause causes the patient to loose the protective function of the ovarian hormones on the bones and the heart.
These are deep-rooted misconceptions. Over 10-15 years ago the treatment of a lot of gynaecological conditions was hysterectomy but not any more
Recent advances in gynaecology means we can now use less invasive methods to treat a lot of these conditions adequately and with minimum risk
Below are instances from practise in my clinic in the last few months:
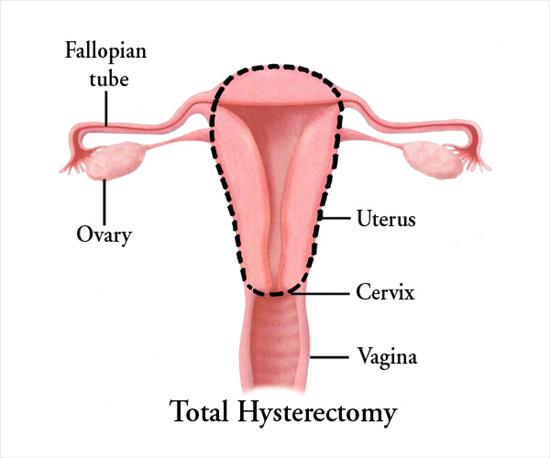
Patient A –had severe menopausal symptoms and came to clinic requesting a hysterectomy. She responded
Brilliantly to hormone replacement therapy and could avoid major surgery and the unnecessary risks and cost.
Patient B– had an endometrial polyp and had been advised hysterectomy. She attended requesting immediate surgery. She had a hysteroscopy and polypectomy as a day surgery procedure instead and was discharged home the same evening with only mild bleeding.
Patient C –demanded immediate hysterectomy for management of her urinary incontinence. She was upset
When she was told that the operation could make her symptoms worse. She was cured with modifying her caffeine intake and with tablets.
Patient D– had heavy periods and was anemic and was struggling with a lack of energy. She had a day case procedure and insertion of a coil, which stopped her periods and made her feel instantly better.
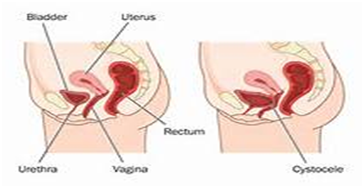
Patient E-had a difficulty with sexual intercourse due to a prolapse and vaginal dryness. She underwent a vaginal procedure to anchor her prolapse and medical treatment for the dryness.
As illustrated with all the above patients, hysterectomy when done for the wrong indications besides not curing the primary symptoms might make the symptoms worse and difficult to treat in future. It is therefore extremely important to consult a gynaecologist with an open mind and discuss your expectation rather than request hysterectomies.

Dr.Vaishnavi- Is a consultant gynaecologist at Kauvery hospital, Chennai.
She is a specialist in advanced and ambulatory gynaecology and minimally invasive gynaecology.
Dr.Vaishnavy also specialises in Urogynaecology and pelvic floor reconstruction surgery.


Give a Reply